The Centers for Medicare and Medicaid Services (CMS) describe DIR fees as “fees, payments, or payment adjustments made after the point-of-sale that change the cost of Part D covered drugs for Part D sponsors or PBMs must be reported to CMS as Direct or Indirect Remuneration (DIR).”
1
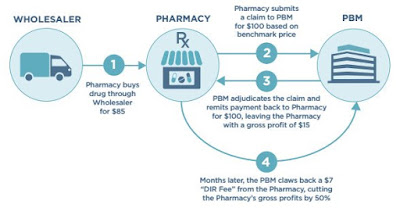 |
| Source: Diplomat Pharmacy |
DIR fees originated in Medicare Part D, however, these fees are now utilized for commercial plans. Pharmacies are charged DIR fees by PBMS after the point of sale. DIR fees may be based on pharmacy performance, ability to participate in a preferred network or as reconciliation between negotiated price and a claim.2 DIR fees have come under scrutiny by pharmacies. According to the White Paper: DIR Fees Simply Explained, DIR fees “create losses in revenue that, at times, may surpass the acquisition cost of the drug itself.” Moreover, certain pharmacy organizations have advocated for DIR fee reform. 3
Based on a survey by the National Community Pharmacy Association (NCPA), a large majority of independent community pharmacy owners do not know what their final reimbursement will be at the point of sale and that it takes 4 to 12 months before they know the final reimbursement figure. 4
For plan sponsors and patients the financial impact of DIR fees are even less transparent. Two big issues surrounding DIR fees for plan sponsors and members, who to a large extent are unaware DIR fees even exist, are:
1) DIR fees hide the true cost of the drug, from the plan sponsor, to the PBMs financial benefit. For example, PBMs might break-even on retail pharamcy network discounts on the front-end only to make up for it on the back-end through DIR fees. PBMs should be negotiating these discounts on behalf of the client then passing these savings onto plan sponsors. At the very least, PBMs should be disclosing their take home on these fees to plan sponsors.
2) Members cost share (i.e. coinsurance) too doesn’t take into account the PBM’s true cost when DIR fees are collected. If these fees were applied at the point-of-sale these plan participants would pay less and in some cases significantly so.
As a first proactive step to manage DIR fees, pharmacies should understand their contract and the various conditions therein. The NCPA DIR Fee FAQ guidance document asserts that pharmacy owners should manage these fees by performing “due diligence when evaluating contracts and make sure you are aware of and understand all of the different terms and conditions contained in your contract including network pharmacy manuals when incorporated by reference into a contract.
Alternately, make sure any contracting entity that might negotiate on your behalf (PSAO) explains to you the parameters of all of your contractual terms.”5
1) https://www.cms.gov/newsroom/fact-sheets/medicare-part-d-direct-and-indirect-remuneration-dir
2) https://www.specialtypharmacytimes.com/news/white-paper-dir-fees-simply-explained/P-1
3) https://www.nacds.org/news/pharmacy-groups-praise-cms-progress-on-dir-fee-reform-to-lower-patients-out-of-pocket-drug-costs/
4) https://www.ncpanet.org/newsroom/news-releases/2018/02/09/ncpa-survey-pharmacy-dir-fees-plague-both-community-pharmacies-and-their-patients
5) http://www.ncpa.co/pdf/dir-faq.pdf

